Last updated: March 25, 2026
Quick Answer: Yes — a qualified dermatologist or minor surgery specialist can safely remove moles using proven techniques like surgical excision or shave removal, usually in a single outpatient visit. Whether you're concerned about a suspicious lesion or simply want a mole removed for cosmetic reasons, professional removal is the safest, most reliable option. Attempting to remove moles at home carries real risks, including infection, scarring, and missed diagnoses.
Key Takeaways
- A dermatologist or trained surgeon should always assess a mole before removal — not just remove it blindly.
- The two most common methods are surgical excision (cutting out the mole and stitching the skin) and shave excision (shaving the mole flush with the skin surface).
- Most mole removals are completed in under 30 minutes as an outpatient procedure.
- Removed moles are typically sent for pathology testing to check for abnormal or cancerous cells.
- Skin cancer rates are rising — over 112,000 Americans are projected to be diagnosed with invasive melanoma in 2026 alone [1].
- Cosmetic mole removal is generally not covered by provincial health insurance in Ontario; medically necessary removal may be covered.
- Choosing a clinic with experienced surgeons and a clear aftercare plan makes a significant difference in outcomes and scarring.
- At-home mole removal products (pens, creams, DIY kits) are not recommended and can delay a critical diagnosis.
What Does It Mean When a Dermatologist Removes a Mole?
When a dermatologist removes a mole, they are performing a minor surgical procedure to excise or shave off a pigmented skin lesion — either because it looks suspicious, is causing discomfort, or the patient wants it gone for cosmetic reasons.
This isn't just a cosmetic snip. A proper mole removal includes:
- Visual and dermoscopic assessment before any cutting begins
- Local anesthetic to numb the area so you feel nothing during the procedure
- Excision or shave removal, depending on the mole's type and depth
- Pathology submission — the removed tissue is sent to a lab for analysis
- Wound closure and aftercare instructions to support healing
The key word here is assessment. A good clinic doesn't just remove what you point at. They evaluate the mole first, because the way a mole looks under a dermatoscope can change everything about how it's treated.
"Think of mole removal less like erasing a mark and more like investigating a clue — the tissue tells a story that a lab can read."
If you're in the Greater Toronto Area and want to understand what the process looks like, the Minor Surgery Center's mole removal overview is a solid starting point.
When Should You See a Dermatologist to Remove a Mole?
You should see a dermatologist or surgeon about a mole if it has changed in appearance, causes symptoms, or simply bothers you. Not every mole needs to come off — but some absolutely should.
The ABCDE rule for suspicious moles
Dermatologists use the ABCDE criteria to flag moles that warrant closer attention:
| Letter | What to Look For |
|---|---|
| A — Asymmetry | One half doesn't match the other |
| B — Border | Edges are ragged, notched, or blurred |
| C — Color | Multiple shades of brown, black, red, white, or blue |
| D — Diameter | Larger than 6mm (about the size of a pencil eraser) |
| E — Evolving | Any change in size, shape, color, or new symptoms like bleeding |
If a mole checks one or more of these boxes, book an appointment promptly. Melanoma diagnoses are projected to rise in 2026, with skin cancer remaining one of the most common cancers in North America [2][3]. Early detection is the single most important factor in a good outcome.
Other valid reasons to have a mole removed
- It catches on clothing or jewelry and bleeds
- It's in a spot that gets irritated regularly (waistband, bra line, collar)
- You simply don't like how it looks — cosmetic removal is completely valid
- A mole appeared after age 30, or you've developed clusters of new moles
For a deeper look at what makes a mole benign versus worth watching, the benign mole explained guide covers the key differences clearly.

How Does a Dermatologist Remove Moles? The Main Methods Explained
A dermatologist removes moles using one of two primary surgical techniques, chosen based on the mole's size, depth, location, and whether it looks suspicious. Both are done under local anesthetic and take under 30 minutes in most cases.
1. Surgical excision (cut and stitch)
This is the most thorough method. The surgeon cuts out the entire mole plus a small margin of surrounding skin, then closes the wound with sutures.
Best for: Moles that are raised, large, deeply pigmented, or show any suspicious features. Also the preferred method when a clean pathology sample is needed.
What to expect: A small scar that fades over several months. Stitches are typically removed within 7–14 days depending on the location.
2. Shave excision
The surgeon uses a fine blade to shave the mole level with the surrounding skin. No deep cutting, no stitches in most cases.
Best for: Raised, benign-looking moles that are primarily a cosmetic concern. Not recommended if the mole looks suspicious, because shave excision may not capture the full depth of the lesion.
What to expect: A small, flat pink mark that usually fades well. Healing is typically faster than with excision.
What about laser or cryotherapy?
Laser removal and cryotherapy (freezing) are sometimes offered for very superficial skin lesions, but they are not standard practice for moles. The main problem: they destroy tissue rather than preserving it for pathology. If a mole turns out to be atypical or cancerous, you've lost the sample needed for diagnosis.
For more on the cryotherapy option and its limitations, see this cryotherapy for mole removal guide.
What Happens to the Mole After It's Removed?
In most cases, the removed mole is sent to a pathology lab for analysis. This is one of the most important parts of the process — and a step that at-home removal methods skip entirely.
A pathologist examines the tissue under a microscope to check for:
- Normal, benign cells (the most common result)
- Atypical or dysplastic cells (mildly abnormal; may need monitoring or re-excision)
- Melanoma or other skin cancers (requires further treatment)
Results typically come back within 1–2 weeks. Your surgeon will contact you with the findings and explain any next steps.
Common mistake: Some patients assume that because a mole "looked fine" to the eye, pathology is unnecessary. Dermoscopy and visual inspection are valuable tools, but they can't replace microscopic tissue analysis. Always choose a clinic that submits removed moles for pathology.
For more on understanding your results, this guide to pathology reports after mole removal breaks down the terminology in plain language.
Does Having a Dermatologist Remove a Mole Hurt?
Mole removal is not painful during the procedure. The only discomfort most patients feel is a brief sting from the local anesthetic injection — after that, the area is numb and you won't feel the excision itself.
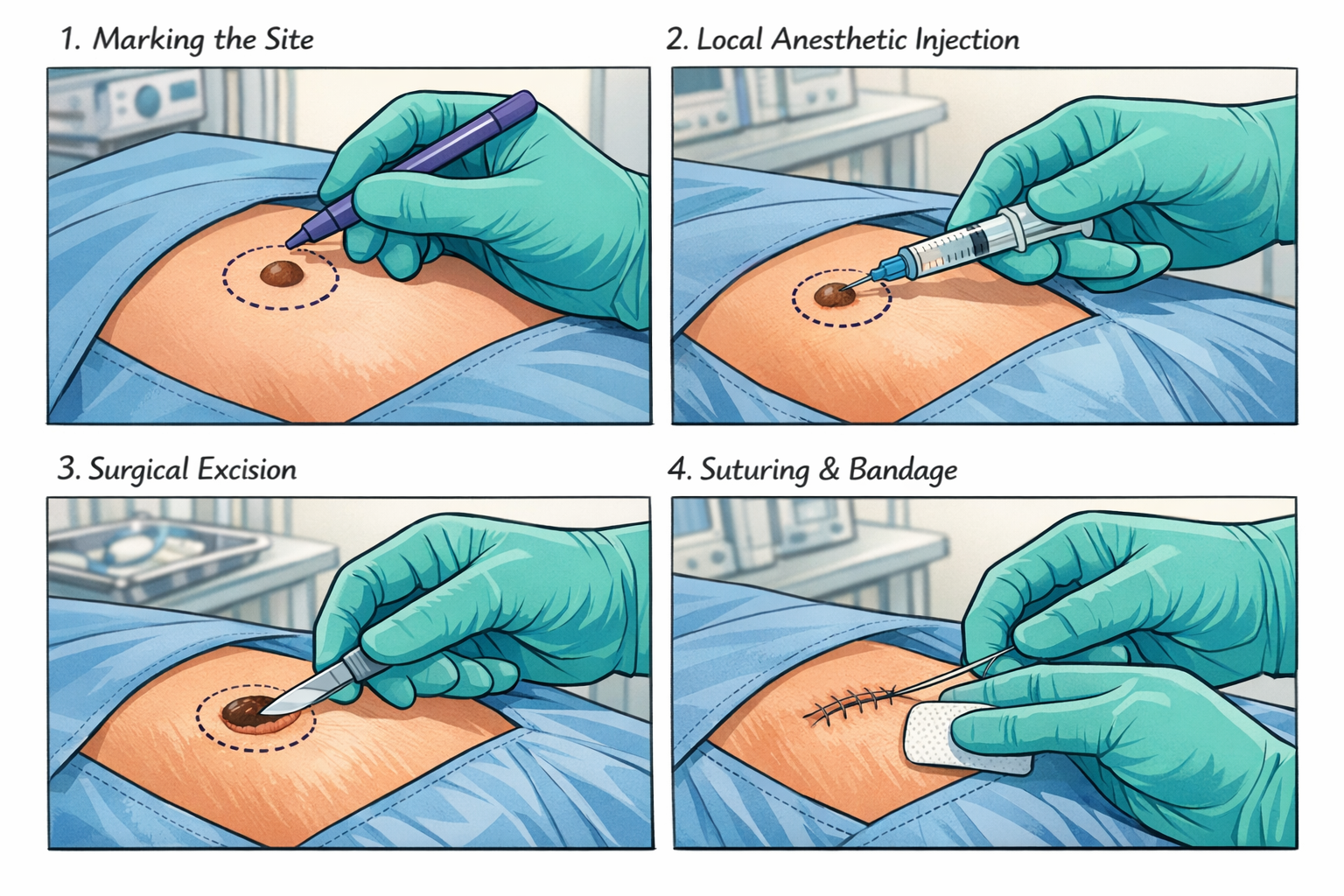
Here's what the experience typically looks like:
- Consultation and assessment — the surgeon examines the mole and discusses the plan with you
- Skin preparation — the area is cleaned and a sterile drape is placed
- Local anesthetic — a small injection numbs the site (this is the "pinch" moment)
- Removal — the procedure takes 5–15 minutes; you feel pressure, not pain
- Closure and dressing — wound is closed and covered; aftercare instructions are given
After the procedure: Some soreness, mild swelling, or tenderness for a few days is normal. Over-the-counter pain relief handles this easily for most people.
For a full breakdown of what to expect, the does mole removal hurt guide answers the most common concerns honestly.
How Much Does It Cost to Have a Dermatologist Remove a Mole in Ontario?
Cost depends on the number of moles, their size and complexity, and the clinic you choose. In Ontario, cosmetic mole removal is not covered by OHIP. Medically necessary removal (where a physician deems it clinically indicated) may be covered, but this varies.
Typical private clinic pricing in the Toronto area (2026 estimates):
| Mole Type / Complexity | Estimated Cost Range |
|---|---|
| Single small mole (shave) | $150 – $300 |
| Single mole (excision + sutures) | $250 – $500 |
| Multiple moles (same visit) | Discounted per additional mole |
| Complex or large lesion | $500+ |
These are general estimates. Pricing varies by clinic, surgeon experience, and whether pathology fees are included.
Pro tip: Many clinics offer a free or low-cost initial consultation. Use it. You'll get a proper assessment, a clear quote, and a chance to ask questions before committing.
To get a personalized estimate, the Minor Surgery Center's cost estimator tool gives you a quick, transparent starting point.
Also worth knowing: removing multiple moles in one visit is often more cost-efficient. See can I remove multiple moles in one visit for details.
How to Choose the Right Clinic to Have a Dermatologist Remove Moles
Not all mole removal clinics are equal. The right choice comes down to surgical experience, pathology practices, and how the clinic communicates with you.
What to look for
- Qualified surgeons — look for board-certified physicians or surgeons, not aestheticians or technicians
- Pathology submission as standard practice — non-negotiable
- Dermoscopy available — modern clinics use dermatoscopes for pre-removal assessment [5]
- Clear pricing and no hidden fees
- Aftercare support — a clinic that answers questions post-procedure
- Real patient reviews — look for consistent feedback on communication, outcomes, and comfort
Red flags to avoid
- Clinics that remove moles without any visual assessment
- Laser-only clinics that don't offer surgical excision
- No mention of pathology testing
- Pressure to book immediately without a consultation
The Minor Surgery Center has performed over 9,000 procedures across the Greater Toronto Area, with clinics in North York, Mississauga, Markham, Brampton, and more. Their experienced surgical team follows a comfort-first approach with a personalised treatment plan for every patient.
What Is Recovery Like After a Dermatologist Removes a Mole?
Recovery from mole removal is straightforward for most people. The goal is to keep the wound clean, protected, and moisturized while the skin heals.
General aftercare timeline
- Days 1–3: Keep the area clean and dry. A small dressing or bandage covers the wound.
- Days 3–7: The wound begins to close. Mild redness and scabbing are normal.
- Week 1–2: Sutures (if used) are removed. The site may still look pink.
- Weeks 4–12: The scar continues to fade. Sun protection on the area is important during this phase.
Scar care
Scarring depends on the removal method, mole size, location, and individual healing. Most people end up with a small, flat scar that fades significantly within 3–6 months.
Options to support scar healing include silicone gel, petroleum jelly, and vitamin E — each with different evidence behind them. For a clear comparison, see best scar care after mole removal.
Edge case: Some people are prone to keloid scarring (raised, thickened scars). If you've had keloid scars before, mention this to your surgeon before the procedure — it affects the technique and aftercare approach.
Frequently Asked Questions About Having a Dermatologist Remove Moles
Q: Can any doctor remove a mole, or does it have to be a dermatologist?
A: Moles can be removed by dermatologists, plastic surgeons, and trained general surgeons or family physicians who perform minor procedures. The key is that the practitioner has surgical training and submits tissue for pathology. A specialist in minor outpatient surgery is an excellent option.
Q: How long does mole removal take?
A: Most mole removals take 10–30 minutes from start to finish, including preparation and wound closure. The excision itself is often done in under 10 minutes.
Q: Will the mole grow back after removal?
A: A mole that is fully excised with clear margins should not grow back. Shave excisions have a slightly higher recurrence rate if any cells remain at the base. See do moles grow back after removal for more detail.
Q: Is it safe to remove a mole at home?
A: No. At-home mole removal pens, creams, and DIY kits are not safe or effective for true moles. They can cause infection, scarring, and — critically — they prevent you from getting a pathology result. If a mole is cancerous, you need to know.
Q: How do I know if my mole removal is covered by OHIP?
A: OHIP covers mole removal only when a physician deems it medically necessary (for example, a lesion with suspicious features). Cosmetic removal is not covered. Ask your clinic to clarify coverage before booking.
Q: What is a dysplastic or atypical mole?
A: An atypical (dysplastic) mole has some abnormal features under the microscope but isn't cancerous. It may need wider re-excision to ensure all abnormal cells are removed. Regular monitoring is recommended for people with multiple atypical moles. Learn more in the atypical moles guide.
Q: Can I get multiple moles removed in one appointment?
A: Yes, in most cases. Removing several moles in one visit is efficient and often more cost-effective. Your surgeon will assess all the moles and prioritize based on concern level.
Q: How soon can I return to normal activities after mole removal?
A: Most people return to desk work the same day or the next day. Strenuous activity or anything that stretches the wound site should be avoided for 1–2 weeks, depending on the location.
Q: Do I need a referral to see a mole removal specialist?
A: Not at private clinics. You can book directly without a referral. This is one of the advantages of outpatient surgical clinics — you get expert outpatient care without the hospital wait times or referral bottleneck.
Q: What's the difference between a mole and a seborrheic keratosis?
A: Seborrheic keratoses are benign, waxy-looking growths that often appear with age. They can look like moles but have a different texture and origin. A dermatologist can distinguish them easily. They're also removable — see seborrheic keratosis removal in Toronto for options.
Q: Is mole mapping worth doing before removal?
A: Mole mapping — photographing and tracking all moles on the body — is a valuable tool for people with many moles or a family history of melanoma. It helps detect changes over time. For Toronto-area options, see the mole mapping clinics guide.
Q: What should I do if a mole bleeds or changes quickly?
A: See a doctor promptly. A mole that bleeds spontaneously, changes rapidly, or develops new symptoms should be assessed without delay — don't wait for a scheduled annual checkup.
Conclusion: Taking the Next Step
Having a dermatologist remove a mole is a safe, quick, and well-established procedure — whether the reason is medical concern or personal preference. The process is straightforward: assessment, anesthetic, removal, pathology, and healing. Most people are back to their normal routine the same day.
What matters most is choosing the right clinic. Look for experienced surgeons, proper pathology practices, and a team that communicates clearly and treats you like a person, not a number.
With melanoma cases rising in 2026 [1][4] and early detection making a measurable difference in outcomes, there's no good reason to delay getting a mole checked. A 20-minute consultation could be one of the most useful appointments you book this year.
Ready to get started?
- Find a mole removal clinic near you
- Use the cost estimator to understand your options
- Browse clinic locations across the GTA
- Read patient reviews from the Minor Surgery Center
You deserve to get back to your life — without a mole that worries you holding you back.
References
[1] Over 112,000 Americans Estimated To Be Diagnosed With Invasive Melanoma In 2026 – https://www.curemelanoma.org/blog/over-112-000-americans-estimated-to-be-diagnosed-with-invasive-melanoma-in-2026
[2] Melanoma Cases Projected To Increase In 2026 – https://www.visionmonday.com/eyecare/health-watch/article/melanoma-cases-projected-to-increase-in-2026
[3] Melanoma Diagnoses Projected To Rise In 2026 – https://www.managedhealthcareexecutive.com/view/melanoma-diagnoses-projected-to-rise-in-2026
[4] Melanoma Cases 2026 Skin Cancer Risk Prevention – https://www.newbeauty.com/melanoma-cases-2026-skin-cancer-risk-prevention/
[5] Dermatology Industry Statistics – https://wifitalents.com/dermatology-industry-statistics/
[6] Skin Cancer Facts – https://www.skincancer.org/skin-cancer-information/skin-cancer-facts/
[7] Stats Skin Cancer – https://www.aad.org/media/stats-skin-cancer
Tags: dermatologist remove moles, mole removal, surgical excision, mole removal Toronto, skin cancer prevention, atypical moles, outpatient mole removal, cosmetic mole removal, mole removal cost Ontario, melanoma detection, minor surgery, shave excision