Last updated: March 25, 2026
Quick Answer: Removing moles is a straightforward outpatient procedure when performed by a qualified surgeon. Most moles are benign and removed for cosmetic reasons or because they cause irritation. The process typically takes 15–30 minutes under local anesthetic, with minimal downtime and a high success rate. If a mole looks unusual or has changed recently, it should be assessed before removal.
Key Takeaways
- Most moles are harmless, but any that change in size, shape, or color should be evaluated promptly.
- The two most common surgical methods are shave excision and excisional surgery (cutting with sutures).
- Laser removal is suitable only for small, flat, confirmed-benign moles.
- A proper clinic sends removed tissue for pathology testing — this is a critical safety step.
- Recovery is usually quick: most patients return to normal activity within 24–48 hours.
- At-home removal methods (creams, pens, DIY kits) are not recommended and can cause scarring or mask a dangerous lesion.
- Cosmetic mole removal is typically not covered by OHIP in Ontario unless there is a medical indication.
- Costs in the Toronto area vary by clinic, mole size, and method — use a mole removal cost estimator to get a clearer picture before booking.
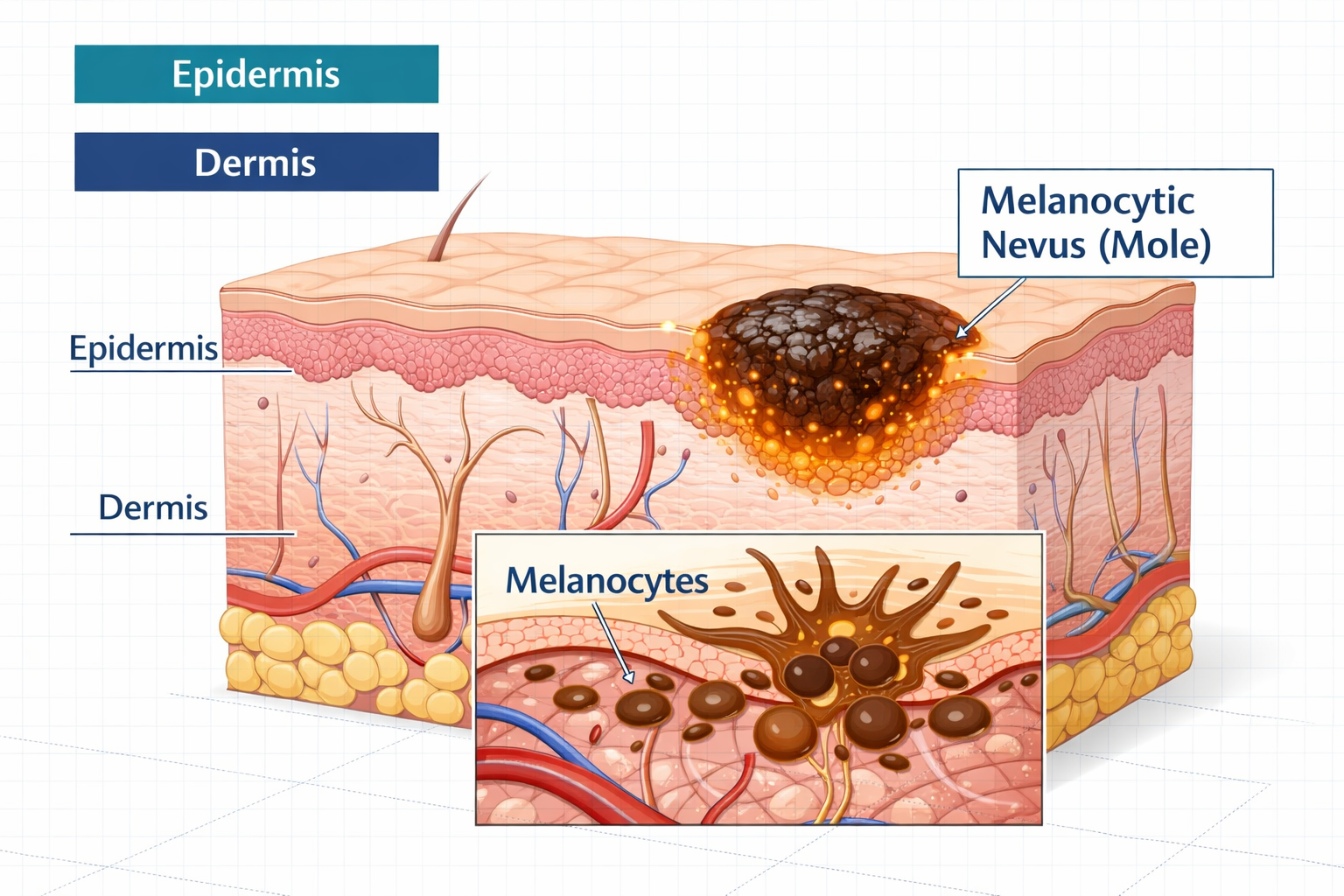
What Is a Mole, and When Should It Be Removed?
A mole (medically called a melanocytic nevus) is a cluster of pigment-producing skin cells called melanocytes. Most people have between 10 and 40 moles by adulthood, and the vast majority are completely harmless.
That said, removing moles becomes worth considering in a few clear situations:
- The mole has changed. New asymmetry, irregular borders, color variation, or growth in diameter are all reasons to get it looked at. This is the ABCDE rule (more on that below).
- It's causing physical discomfort. Moles on the neck, waistband, or underarm can catch on clothing or get nicked while shaving.
- You simply don't want it there. Cosmetic removal is entirely valid. Many patients choose to remove moles on the face, chest, or other visible areas for personal reasons.
- A dermatologist or doctor has flagged it. If a professional has recommended removal or biopsy, don't delay.
"A mole that's been the same your whole life is rarely a concern. A mole that's new or changing is the one worth watching."
Common mistake: Waiting too long because a mole "doesn't look that bad." If it's changed noticeably over a few weeks or months, book an assessment sooner rather than later.
How Do Doctors Assess a Mole Before Removing It?
Before any removal, a qualified clinician evaluates the mole using a structured checklist. The most widely used framework is the ABCDE rule:
| Letter | What It Stands For | What to Look For |
|---|---|---|
| A | Asymmetry | One half doesn't match the other |
| B | Border | Edges are ragged, notched, or blurred |
| C | Color | Multiple shades of brown, black, red, or white |
| D | Diameter | Larger than 6mm (about the size of a pencil eraser) |
| E | Evolving | Any change in size, shape, color, or new symptoms like bleeding |
A clinician may also use a dermatoscope — a handheld magnifying tool with polarized light — to examine the mole's internal structure before deciding on the best approach.
If there's any concern about an atypical mole, the tissue removed during the procedure is sent to a pathology lab for analysis. This step is non-negotiable at a reputable clinic.
Edge case: Some moles that look perfectly normal to the naked eye can show atypical features under dermoscopy. This is exactly why professional assessment matters more than a self-check alone.
What Are the Main Methods for Removing Moles?
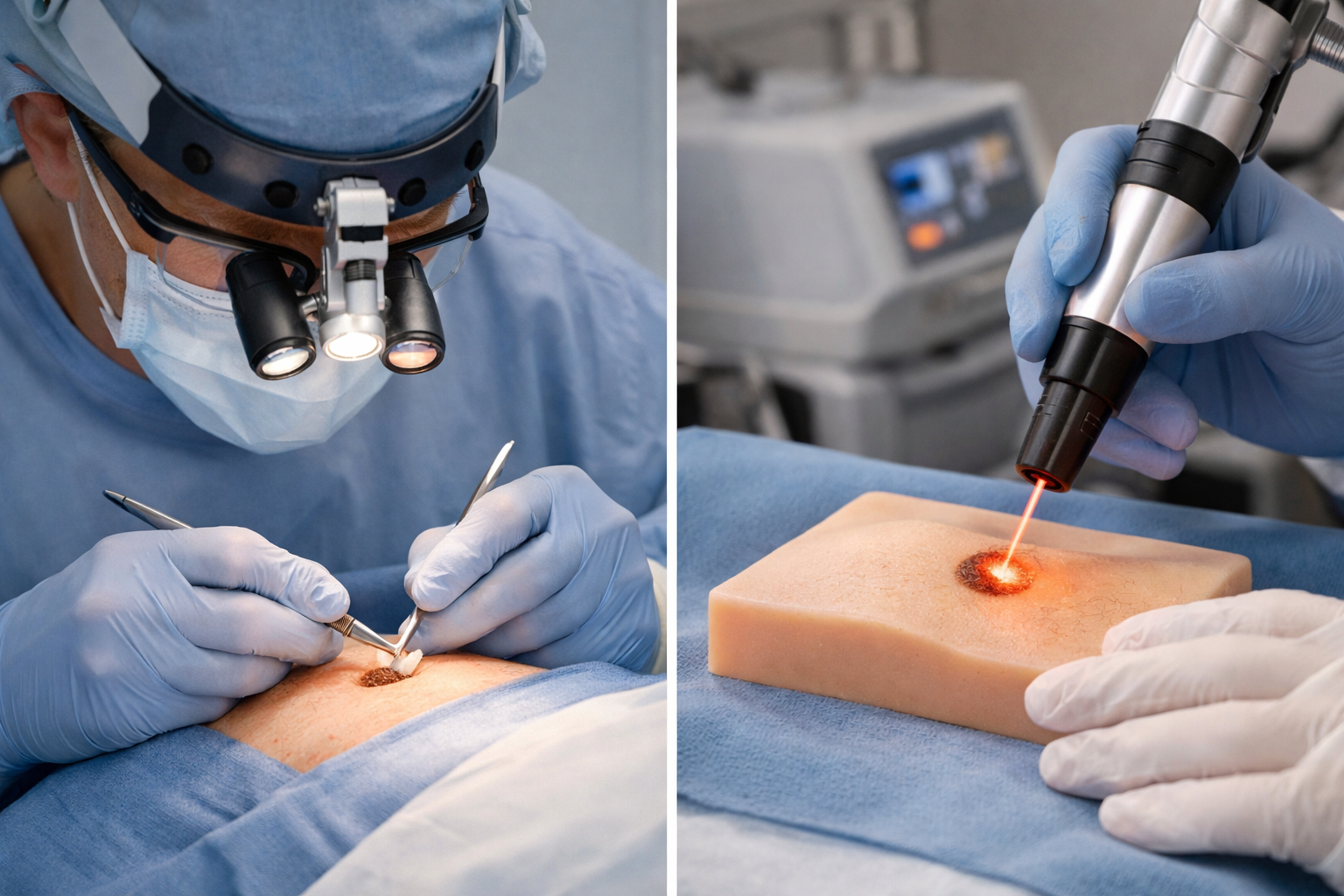
There are several established techniques for removing moles. The right method depends on the mole's size, depth, location, and whether pathology testing is needed.
Shave Excision
The surgeon uses a small blade to shave the mole flush with the surrounding skin. This works well for raised moles that don't extend deep into the dermis.
- No sutures needed in most cases
- Heals within 1–3 weeks
- Leaves a flat, faint mark that fades over time
- Tissue can still be sent for pathology
Excisional Surgery (Punch or Elliptical Excision)
The surgeon cuts the entire mole out, including a small margin of surrounding tissue, and closes the wound with sutures. This is the preferred method when:
- The mole is flat or deeply pigmented
- There's any concern about abnormal cells
- A complete tissue sample is needed for pathology
Recovery takes slightly longer (sutures are removed in 5–14 days depending on location), but this method offers the most thorough removal. The experienced surgical team at The Minor Surgery Center has performed over 9,000+ procedures using this approach.
Laser Removal
A focused laser beam breaks down pigment cells. This is only appropriate for:
- Small, flat, confirmed-benign moles
- Moles in cosmetically sensitive areas where minimal scarring is a priority
Important limitation: Laser removal does not produce a tissue sample, so pathology testing is not possible. For any mole with uncertain features, laser is not the right choice. Learn more about what to expect with cosmetic mole removal.
Cryotherapy
Liquid nitrogen freezes and destroys the mole tissue. It's more commonly used for skin tags or warts, and is generally not recommended as a first-line option for moles because it doesn't allow pathology testing and may not remove deeper cells. Read a full breakdown of cryotherapy for mole removal.
Choose excisional surgery if: The mole is flat, has irregular features, or you want the peace of mind that comes with a pathology report.
Choose shave excision if: The mole is raised, clearly benign, and you want the fastest recovery.
What Does the Mole Removal Process Actually Look Like?

For most patients, the entire process from consultation to healed skin takes about 4–6 weeks. Here's what to expect at each stage.
Step 1: Consultation and Assessment
A surgeon examines the mole, reviews your medical history, and recommends the best removal method. This is also when you can ask questions, discuss scar expectations, and understand the cost. The Minor Surgery Center offers a personalised treatment plan for every patient.
Step 2: The Procedure
- Local anesthetic is injected to numb the area. Most patients feel a brief sting, then nothing.
- The surgeon removes the mole using the agreed method. This typically takes 15–30 minutes.
- The wound is cleaned and dressed.
- If excisional surgery was performed, sutures are placed.
Step 3: Pathology (If Applicable)
The removed tissue is sent to a lab. Results typically come back within 1–2 weeks. You'll be contacted if anything requires follow-up. For help understanding what your results mean, see this guide to demystifying your pathology report after mole removal.
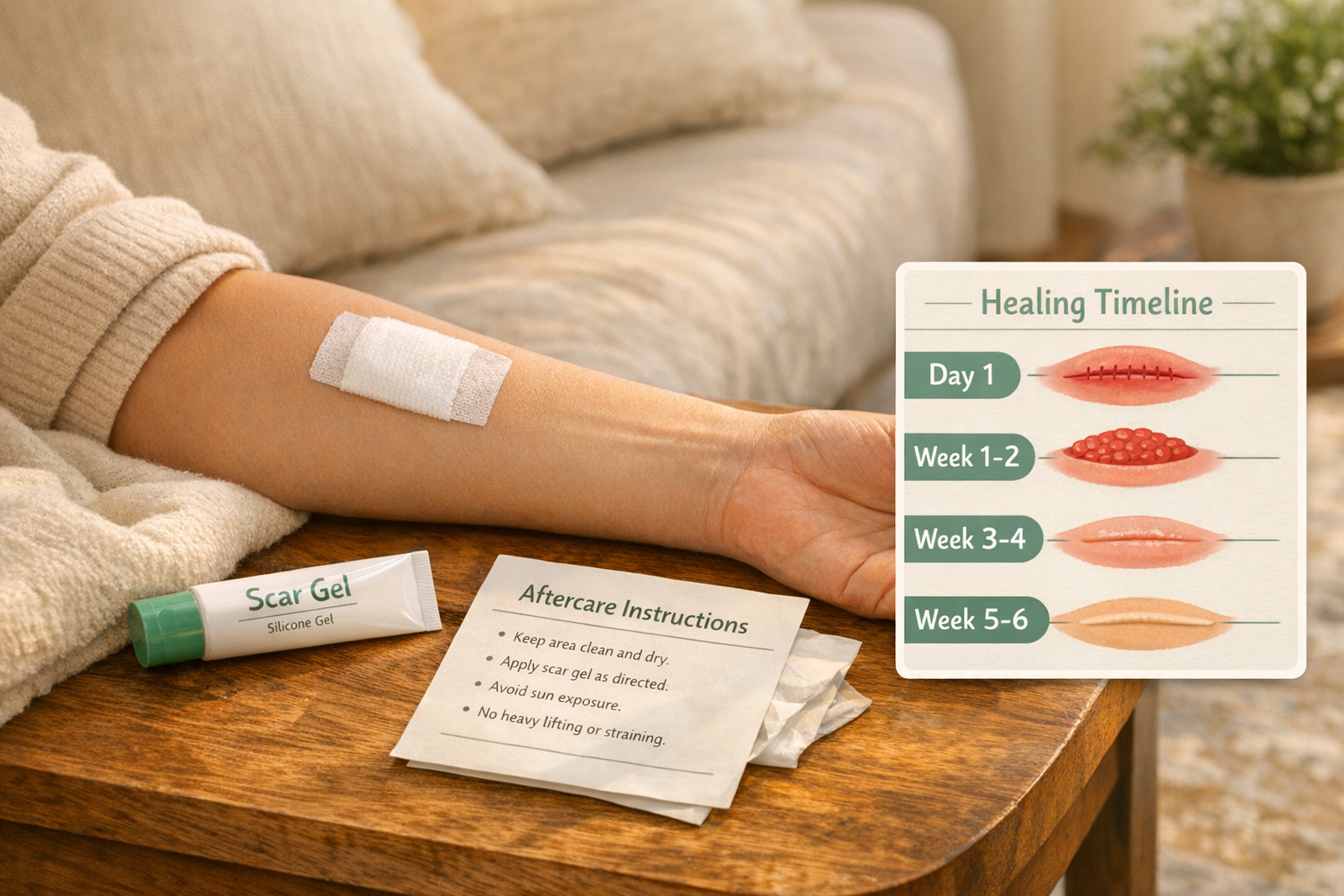
Step 4: Healing and Aftercare
- Keep the area clean and covered for the first few days.
- Avoid sun exposure on the healing site.
- Apply recommended ointments or silicone gel to minimize scarring.
- Attend any follow-up appointments for suture removal.
For a detailed breakdown of scar management options, see best scar care after mole removal.
Is Removing Moles Safe? What Are the Risks?
When performed by a qualified surgeon in a proper clinical setting, mole removal is very safe. Serious complications are rare. That said, it's worth knowing what the realistic risks are.
Common, minor side effects:
- Temporary redness, swelling, or bruising around the site
- A small scar (all methods leave some trace)
- Temporary skin discoloration, especially in darker skin tones
Less common risks:
- Infection (minimized with proper aftercare)
- Incomplete removal, which may require a second procedure
- Nerve sensitivity or numbness near the site (usually temporary)
The bigger risk of NOT removing a suspicious mole: A mole that is left unchecked and turns out to be melanoma is far more dangerous than any minor surgical risk. Early detection and removal of atypical moles dramatically improves outcomes.
A common concern is whether removing a mole can cause cancer. The short answer is no — but it's worth reading the full explanation at does removing a mole cause cancer.
Comfort-first approach: At The Minor Surgery Center, local anesthetic is used for every procedure. Most patients are surprised by how comfortable the experience is. If you're anxious about pain, read does mole removal hurt for an honest, detailed answer.
How Much Does Mole Removal Cost in Toronto in 2026?
Mole removal costs in the Toronto area vary depending on the method, the number of moles, and the clinic. Here's a general overview:
| Method | Typical Cost Range (Toronto, 2026) |
|---|---|
| Shave excision (single mole) | $150 – $350 |
| Excisional surgery (single mole) | $250 – $500 |
| Multiple moles (same visit) | Often discounted per additional mole |
| Laser removal | $150 – $400 per session |
OHIP coverage: In Ontario, mole removal is covered by OHIP only when there is a documented medical reason (such as suspected malignancy). Cosmetic removal is typically an out-of-pocket expense.
Good news: Removing multiple moles in a single visit is usually more cost-effective than separate appointments. Learn more about removing multiple moles in one visit.
Use The Minor Surgery Center's free cost estimator tool to get a personalized estimate based on your specific situation.
What Are the Latest Advances in Mole Removal?
The field of dermatology and skin surgery continues to evolve. Here are some of the most relevant developments as of 2026.
Surface Radiotherapy (SRT) for Non-Melanoma Skin Cancer
For patients diagnosed with non-melanoma skin cancers (like basal cell carcinoma or squamous cell carcinoma), Surface Radiotherapy (SRT) has emerged as a strong non-surgical alternative. In 2026, new CMS standards were implemented that classify SRT as a standalone treatment modality, with recurrence-free rates reported at 99%+ across all stages [5].
SRT does not require surgery, anesthesia, or follow-up reconstruction — it consists of short, targeted treatment sessions [5]. This is particularly relevant for older patients or those who are not good surgical candidates.
Gene Silencing Therapy for Giant Congenital Moles
For a rare but serious condition called congenital melanocytic naevus syndrome (CMN) — where children are born with moles covering up to 80% of their body — researchers at the Francis Crick Institute and Great Ormond Street Hospital have developed a promising genetic therapy [2].
The treatment uses a silencing RNA to target the mutated NRAS gene responsible for the abnormal mole growth. In laboratory and animal tests, it successfully triggered the self-destruction of mole cells, with NRAS gene expression reduced within just 48 hours [3]. Human clinical trials were expected to begin within a few years of the June 2024 announcement [2].
This research won't change everyday mole removal for most patients, but it represents a significant step forward for those with severe congenital conditions [1].
AI-Assisted Dermoscopy
Artificial intelligence tools are increasingly being used to assist clinicians in analyzing dermoscopy images for early signs of melanoma. These tools don't replace expert judgment but can flag borderline cases for closer review [6].
What Should You Avoid When Removing Moles?
This is where many people go wrong. Here are the most important things to avoid.
❌ At-home removal methods
Mole removal creams, DIY pens, and home kits are not safe or effective. They can cause chemical burns, permanent scarring, and — critically — they destroy the tissue needed for pathology testing. If a mole turns out to be cancerous, that missed diagnosis can have serious consequences. Read the full breakdown on mole removal creams and mole removal pens before considering either option.
❌ Choosing a clinic that skips pathology
Any clinic that removes a mole without offering to send it for pathology testing is cutting a critical corner. Always ask whether the tissue will be analyzed.
❌ Ignoring a changing mole
Waiting months to have a changing mole assessed because it "doesn't seem urgent" is one of the most common — and potentially dangerous — mistakes. When in doubt, book an assessment.
❌ Sun exposure on a healing wound
UV exposure on a fresh scar significantly increases the risk of permanent discoloration. Cover healing sites with SPF 50+ or a bandage when outdoors.
Where Can You Get Moles Removed in the Toronto Area?
The Minor Surgery Center offers expert outpatient care for mole removal across multiple locations in the Greater Toronto Area and beyond. Each clinic is staffed by board-certified surgeons who specialize in minimally invasive solutions for skin conditions.
Here are the available clinic locations:
- Downtown Toronto Mole & Cyst Removal
- Mississauga Mole, Cyst & Skin Tag Removal
- Scarborough Mole, Cyst & Skin Tag Removal
- Markham Mole, Cyst & Minor Surgery
- Oakville Mole, Cyst & Skin Tag Removal
- Brampton Mole, Cyst & Skin Tag Removal
- North York Mole, Cyst & Skin Tag Removal
- Newmarket Mole, Cyst & Skin Tag Removal
- Barrie Mole & Cyst Removal
Each location offers the same standard of safe and efficient surgery, with no hospital wait times and a clear, transparent process from start to finish.
Frequently Asked Questions About Removing Moles
Q: How long does mole removal take?
Most procedures take 15–30 minutes from start to finish. The actual removal is often completed in under 10 minutes; the rest is preparation and wound care.
Q: Will mole removal leave a scar?
All methods leave some trace, but scars typically fade significantly over 6–12 months. Proper aftercare (silicone gel, sun protection) makes a meaningful difference in the final appearance.
Q: Can I remove more than one mole in the same appointment?
Yes. Removing multiple moles in one visit is common and usually more cost-effective. See can I remove multiple moles in one visit for details.
Q: Does mole removal hurt?
The local anesthetic injection causes a brief sting. After that, the area is numb and most patients feel only mild pressure. Post-procedure soreness is usually mild and manageable with over-the-counter pain relief.
Q: Do I need a referral to have a mole removed?
At The Minor Surgery Center, a referral is not always required. Contact the clinic directly to confirm the process for your specific situation.
Q: How do I know if my mole needs to be removed urgently?
If your mole is bleeding, growing rapidly, itching persistently, or has changed noticeably in a short period, book an assessment promptly rather than waiting for a routine appointment.
Q: Can moles grow back after removal?
It's possible, especially with shave excision if some cells remain at the base. Excisional surgery with a clear margin has a lower recurrence rate. If a mole does return, it should be re-evaluated.
Q: Is it safe to remove a mole during pregnancy?
Elective mole removal is generally deferred until after delivery unless there is a medical concern. Hormonal changes during pregnancy can affect moles, so monitoring is usually recommended first.
Q: What is the difference between a mole and a skin tag?
A mole is a pigmented cluster of melanocytes. A skin tag is a small, soft flap of excess skin, usually flesh-colored. Both can be removed, but they are different structures requiring slightly different approaches.
Q: Are at-home mole removal kits safe?
No. They are not recommended. They can cause burns, scarring, and infection, and they prevent the tissue from being tested for cancer cells. Always see a qualified clinician.
Conclusion
Removing moles is one of the most common and straightforward minor surgical procedures available. Whether the goal is peace of mind, comfort, or cosmetic improvement, the process is safe, quick, and well-tolerated when done by an experienced surgical team in a proper clinical setting.
The key steps are simple: get the mole assessed by a qualified clinician, choose the right method for your specific mole, and follow through with aftercare and pathology review if applicable.
Your next steps:
- Check your moles using the ABCDE rule. If anything concerns you, don't wait.
- Book a consultation at a Minor Surgery Center location near you — no hospital, no long wait lists.
- Use the cost estimator to understand pricing before your appointment.
- Ask about pathology at your consultation — any reputable clinic will offer it.
Getting a mole removed shouldn't feel like a big deal. With the right clinic and the right approach, it usually isn't. You can get back to your life quickly, with one less thing to worry about.
References
[1] Potential Mole Reversal Therapy Rare – https://medicalxpress.com/news/2024-06-potential-mole-reversal-therapy-rare.html
[2] Science Daily – https://www.sciencedaily.com/releases/2024/06/240617173527.htm
[3] Potential Life Transforming Mole Reversal Therapy Shown Rare Condition – https://www.ucl.ac.uk/news/2024/jun/potential-life-transforming-mole-reversal-therapy-shown-rare-condition
[4] The Latest Advances In Mole Removal Techniques – https://www.rexburgskincare.com/the-latest-advances-in-mole-removal-techniques
[5] 2026 CMS Non-Invasive Skin Cancer Treatment – https://sensushealthcare.com/2026-cms-non-invasive-skin-cancer-treatment/
[6] Top Advances Dermatology 2026 – https://www.london-dermatology-centre.co.uk/blog/top-advances-dermatology-2026/
Tags: mole removal, removing moles, mole excision, cosmetic mole removal, skin mole treatment, mole removal Toronto, outpatient surgery, minor surgery, mole assessment, ABCDE rule, mole removal cost, benign mole