
Most people spend more time researching a new phone than they do understanding what happens to their skin after mole removal — yet the healing process is where the real outcome is decided. Whether your mole was removed for cosmetic reasons or out of a medical precaution, knowing exactly what to expect during each of the mole removal healing stages can mean the difference between a barely-visible scar and one that draws attention for years.
At The Minor Surgery Center (TMSC), our board-certified plastic surgeons perform mole removals daily across our Toronto, Oakville, Vaughan, and Mississauga clinics — often as same-day, no-referral procedures. We've guided thousands of patients through recovery, and this guide distills everything we've learned into one practical, honest resource.
Key Takeaways
- ✅ Healing is a staged process — most patients see significant improvement within 6 weeks, with final scar maturation taking up to 12 months.
- ✅ The first 72 hours are the most critical — proper wound care in this window sets the foundation for minimal scarring.
- ✅ Keeping the wound moist (not wet) accelerates healing — contrary to the old "let it air out" advice, moist wound healing is now the gold standard.
- ✅ Sun protection is non-negotiable — UV exposure on a healing scar is one of the top causes of permanent discolouration.
- ✅ Procedure type matters — shave excision, punch excision, and surgical excision each follow slightly different healing timelines.
Understanding the Two Main Types of Mole Removal
Before diving into the timeline, it helps to know that not all mole removals heal the same way. The technique your surgeon uses directly affects how your skin recovers.
| Removal Method | How It Works | Typical Healing Time | Sutures Required? |
|---|---|---|---|
| Shave Excision | Mole shaved flush with skin surface | 1–3 weeks | No |
| Punch Excision | Small circular tool removes mole + margin | 2–4 weeks | Sometimes |
| Surgical Excision | Mole cut out with scalpel, elliptical incision | 4–8 weeks | Yes |
| Laser Removal | Laser energy breaks down pigment | 1–3 weeks | No |
"The goal of any mole removal isn't just to remove the mole — it's to leave behind the least possible evidence that it was ever there."
— TMSC Board-Certified Plastic Surgeon
At TMSC, our surgeons select the most appropriate technique based on the mole's size, depth, location, and your skin type. This individualized approach is a key reason our patients consistently achieve excellent cosmetic outcomes.
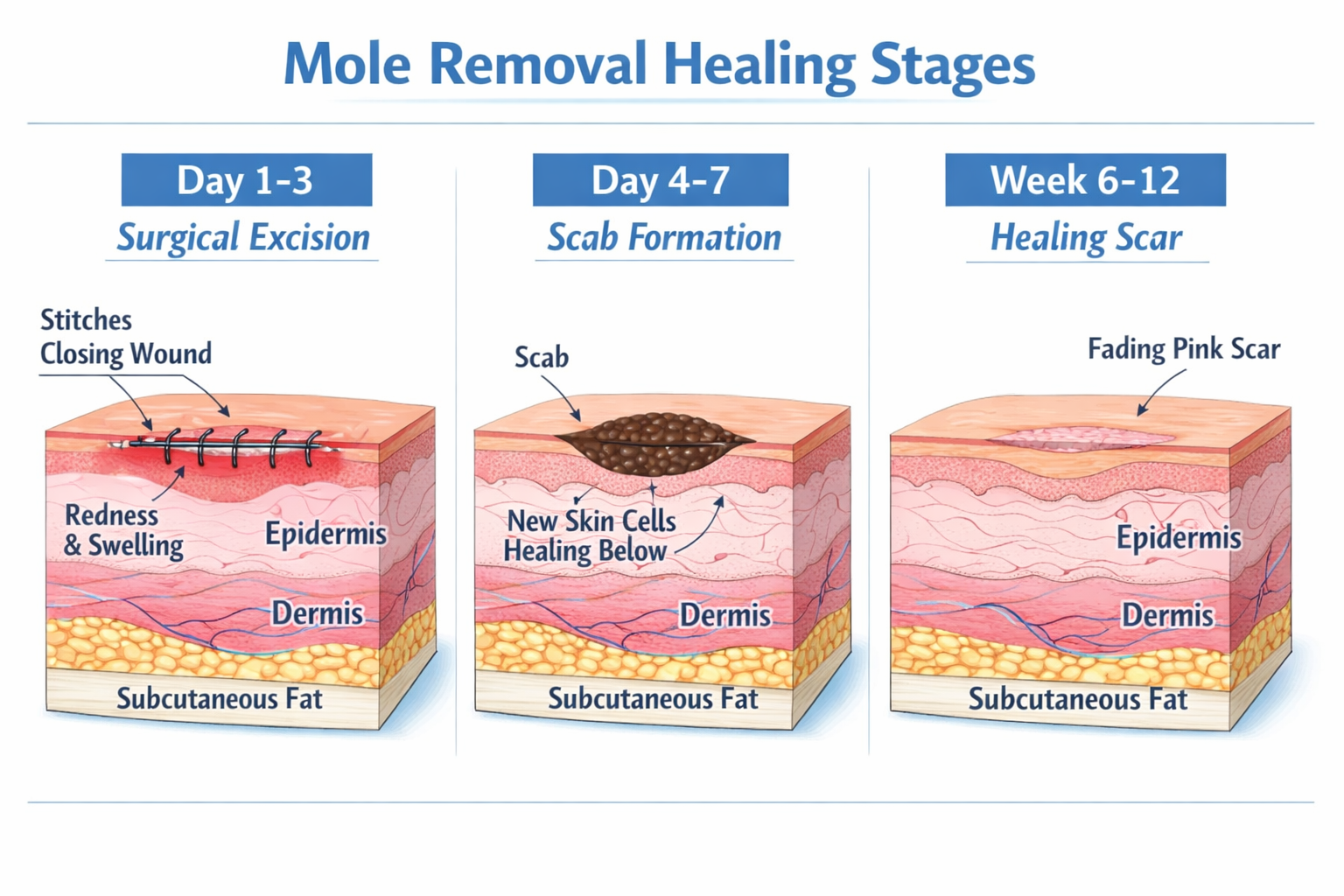
The Mole Removal Healing Stages: A Day-by-Day, Week-by-Week Timeline
Understanding the mole removal healing stages in sequence removes the anxiety of wondering "Is this normal?" at every step. Here's exactly what to expect.
🩹 Days 1–3: The Acute Inflammatory Phase
This is your body's emergency response kicking in — and it's supposed to look a little alarming.
What you'll notice:
- Redness, swelling, and mild warmth around the wound site
- Light bleeding or oozing (especially in the first 24 hours)
- Tenderness or a mild stinging sensation
- A small scab or crust beginning to form
What's happening under the skin:
Your immune system is flooding the area with white blood cells to fight potential infection and begin debris cleanup. Blood vessels dilate, which causes the redness and warmth. Platelets rush in to form a clot and seal the wound.
What to do:
- Keep the wound covered with a clean, non-stick dressing
- Apply a thin layer of antibiotic ointment (like Polysporin) as directed
- Avoid getting the area wet for the first 24–48 hours
- Do NOT pick at any forming scab
- Take over-the-counter pain relief if needed (acetaminophen is preferred over ibuprofen, which can thin the blood)
⚠️ When to call your clinic: Increasing redness spreading beyond the wound edges, significant swelling, pus, or fever above 38°C (100.4°F) — these may indicate infection.
🩹 Days 4–7: Proliferation Begins
The dramatic inflammation starts to calm down, and your body shifts into active rebuilding mode.
What you'll notice:
- Redness begins to fade at the wound edges
- A firmer scab or crust has formed
- The area may feel itchy — this is a positive sign of healing
- If sutures were placed, they remain intact and the skin around them may look slightly puckered
What's happening under the skin:
Fibroblasts (specialized repair cells) are now producing collagen — the structural protein that will form new skin. New blood vessels are growing into the wound (a process called angiogenesis). The wound edges are slowly contracting.
What to do:
- Continue daily wound care: gently clean with saline or mild soap, pat dry, apply ointment, re-dress
- Resist the urge to scratch — itching means nerves are regenerating, which is good
- Avoid strenuous exercise that causes sweating near the wound
- Stay out of pools, hot tubs, and natural bodies of water
- Keep the area out of direct sunlight entirely
💡 Pro tip from our surgeons: Moist wound healing — keeping the site lightly coated with ointment rather than letting it dry out — has been shown in clinical research to speed healing and reduce scarring. Don't let the wound "breathe" by leaving it uncovered.
🩹 Week 2: Suture Removal & Surface Closure
For most surgical excisions, sutures are removed between Days 7–14, depending on the location of the wound (facial sutures come out sooner; body sutures later).
What you'll notice:
- The wound surface may appear closed or nearly closed
- A pink or red line where the incision was made
- Slight firmness or raised texture along the scar line — this is normal
- Residual itching as nerve endings continue to regenerate
What's happening under the skin:
Collagen production is in full swing. The new scar tissue is immature — it has more collagen than it needs and the fibres are disorganized. This is why new scars often feel firm and look raised and pink.
What to do:
- Attend your follow-up appointment for suture removal (TMSC schedules this automatically)
- Begin silicone gel or silicone sheeting if your surgeon recommends it — this is one of the most evidence-backed tools for scar management
- Start gentle scar massage only after your surgeon confirms the wound is fully closed (typically after suture removal)
- Introduce SPF 30+ sunscreen to the area once the wound is fully closed
🩹 Weeks 3–6: Active Scar Remodelling
This phase is where most patients start to feel genuinely optimistic — or, if they haven't followed aftercare instructions, start to worry.
What you'll notice:
- The scar gradually flattens
- Colour shifts from bright red/pink toward a lighter pink
- Firmness begins to soften
- Some patients notice the scar is still slightly raised — this is still within normal range
What's happening under the skin:
The body is reorganizing and cross-linking collagen fibres, making the scar stronger and more structured. Blood vessel density in the scar begins to decrease, which is why the colour fades. The scar is still actively remodelling — it's not "done" yet.
What to do:
- Apply silicone gel twice daily (morning and evening)
- Perform scar massage for 5–10 minutes daily using gentle circular pressure
- Apply broad-spectrum SPF 50 every morning — UV exposure can permanently darken a healing scar
- Avoid activities that stretch or stress the scar (e.g., heavy lifting if the mole was on the trunk)
- Maintain a healthy diet rich in vitamin C and zinc, which support collagen synthesis
🩹 Weeks 6–12+: Maturation & Final Results
What you'll notice:
- The scar continues to fade — often becoming significantly lighter than it appeared at Week 3
- Texture becomes smoother and flatter
- The scar may still be slightly pink at 3 months; this is completely normal
- Final scar appearance is typically not assessed until 12 months post-procedure
What's happening under the skin:
Collagen remodelling continues slowly. The scar tissue gradually becomes more organized and less vascular. Mature scar tissue is typically white or skin-coloured and flat.
What to do:
- Continue sun protection indefinitely — healed scars remain sensitive to UV
- If the scar is raised (hypertrophic) or spreading (keloid), discuss options with your surgeon — treatments like steroid injections or laser therapy may be recommended
- Be patient: most scars look dramatically better at 6 months than they do at 6 weeks
📌 Important: Keloid formation is more common in certain skin types and body locations (chest, shoulders, earlobes). If you have a history of keloids, tell your surgeon before your procedure so a prevention plan can be put in place.
Practical Aftercare Tips for Optimal Healing
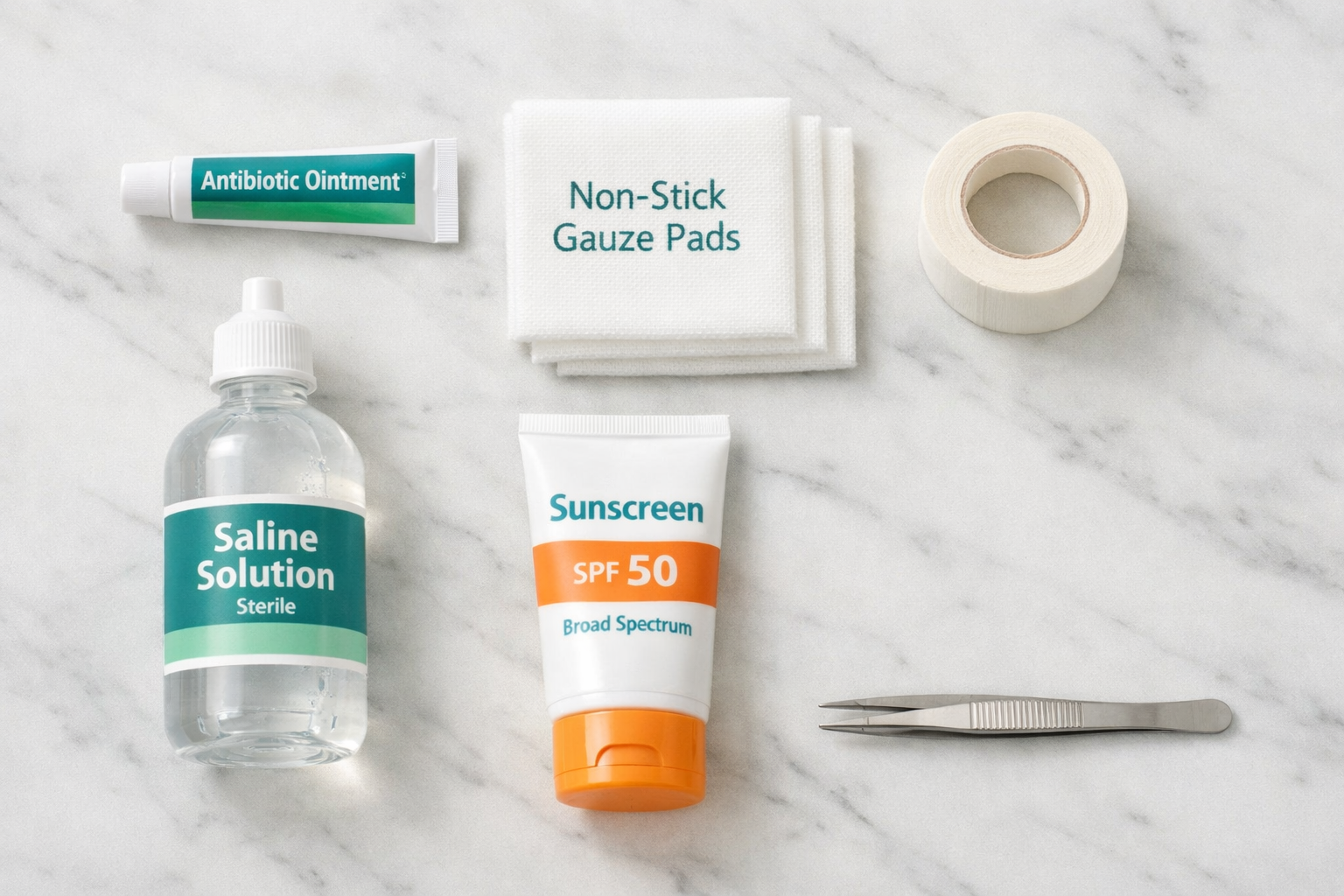
These are the specific, actionable steps that make the biggest difference in your healing outcome. Think of this as your daily checklist.
Your Daily Wound Care Routine (First 2 Weeks)
- Wash your hands thoroughly before touching the wound
- Gently cleanse the area with saline solution or mild, fragrance-free soap
- Pat dry with a clean gauze pad — never rub
- Apply a thin layer of antibiotic ointment (Polysporin or Vaseline if no infection risk)
- Cover with a non-stick sterile dressing
- Repeat once or twice daily, or whenever the dressing gets wet or dirty
The 6 Rules That Protect Your Results
| Rule | Why It Matters |
|---|---|
| 🚫 No sun exposure on the wound | UV rays permanently darken new scar tissue |
| 🚫 No swimming for 2–3 weeks | Waterborne bacteria can cause infection |
| 🚫 No picking or scratching | Disrupts collagen formation, worsens scarring |
| ✅ Keep it moist | Moist healing reduces scab thickness and scar depth |
| ✅ Use silicone products | Clinically proven to flatten and fade scars |
| ✅ Attend all follow-ups | Allows early detection of complications |
Nutrition That Supports Skin Healing
Your skin heals from the inside out. During recovery, prioritize:
- Vitamin C (citrus, bell peppers, strawberries) — essential for collagen synthesis
- Zinc (pumpkin seeds, lean meat, legumes) — supports tissue repair and immune function
- Protein (eggs, fish, chicken, tofu) — provides amino acids for new cell construction
- Hydration — well-hydrated skin heals faster and scars less visibly
What's Normal vs. What's Not: A Quick Reference
Knowing the difference between expected healing and a complication gives you peace of mind and helps you act quickly when needed.
✅ Normal Healing Signs
- Mild redness, swelling, and tenderness in the first 3–5 days
- Itching during Week 1–3
- A firm, slightly raised pink scar in the first 4–8 weeks
- Gradual fading of scar colour over 3–12 months
🚨 Signs to Contact Your Clinic
- Increasing redness that spreads beyond the wound edges after Day 3
- Pus or cloudy discharge from the wound
- Fever above 38°C (100.4°F)
- Wound edges separating (dehiscence)
- Excessive or worsening pain after the first 48 hours
- A rapidly growing, raised scar (possible keloid formation)
TMSC patients have direct access to their care team throughout recovery. You're never left guessing.
Why Procedure Quality Directly Affects Healing
Here's something that doesn't get talked about enough: how well your mole removal heals is largely determined before the procedure even begins.
The skill of your surgeon, the technique chosen, the precision of the incision, and the quality of suture closure all set the ceiling for your healing outcome. A poorly executed shave excision can leave a depressed scar. Sutures placed under too much tension can cause a wide, stretched scar. Inadequate depth of excision can result in mole recurrence.
This is why choosing an experienced, board-certified plastic surgeon matters — not just for safety, but for aesthetics.
At TMSC, every mole removal is performed by a board-certified plastic surgeon with extensive experience in both medical and cosmetic skin procedures. Our surgeons use fine, layered closure techniques that minimize tension on the skin surface — a key factor in producing narrow, flat scars.
Frequently Asked Questions About Mole Removal Healing Stages
Q: How long until I can wear makeup over the removal site?
A: Wait until the wound is fully closed — typically 10–14 days for surgical excisions. Use mineral-based, fragrance-free products initially.
Q: Will the scar be visible forever?
A: Most scars become very faint or nearly invisible over 12 months, especially with proper aftercare. Location, skin tone, and technique all play a role.
Q: Can I exercise after mole removal?
A: Light walking is fine from Day 1. Avoid sweating near the wound or activities that stretch the scar for at least 2 weeks. Ask your surgeon for specific guidance based on where your mole was located.
Q: When will I know the final result?
A: Surgeons typically assess final scar outcome at the 12-month mark. Most patients are pleasantly surprised by how much improvement occurs between months 3 and 12.
Q: What if my scar becomes raised or thickened?
A: This may indicate a hypertrophic scar or keloid. Contact your TMSC surgeon — early intervention with silicone therapy, steroid injections, or laser treatment produces the best results.
Book Your Free Consultation at The Minor Surgery Center

If you've been putting off mole removal because you weren't sure what recovery would look like — now you know. The mole removal healing stages are manageable, predictable, and well within your control when you have the right care team guiding you.
Here's what makes TMSC different:
- 🏥 No referral needed — book directly, no GP visit required
- ⚡ Same-day procedures available — walk in, have it done, walk out
- 👨⚕️ Board-certified plastic surgeons at every location
- 📍 Four convenient locations — Toronto, Oakville, Vaughan, and Mississauga
- 💬 Free consultations — understand your options before committing
- 🔬 All removed moles sent for pathology — your health is never left to chance
Whether you have a mole that concerns you medically, one that bothers you cosmetically, or simply one you've been meaning to deal with for years — TMSC makes the process straightforward, safe, and stress-free.
Conclusion
The mole removal healing stages follow a reliable biological sequence: acute inflammation in Days 1–3, active repair through Days 4–14, collagen remodelling from Weeks 3–6, and gradual scar maturation through 12 months. Each stage has a clear set of expectations and a specific set of actions that support the best possible outcome.
The most important things you can do are: protect the wound in the early days, keep it moist, shield it from the sun relentlessly, and choose a skilled surgeon who sets you up for success from the first incision.
Your actionable next steps:
- 📞 Book your free consultation at TMSC — no referral, no waiting
- 📋 Ask your surgeon which removal technique is right for your mole and what your specific healing timeline will look like
- 🛒 Prepare your aftercare kit before your procedure: non-stick dressings, antibiotic ointment, saline, SPF 50, and silicone gel
- 📅 Mark your calendar for your follow-up appointment and commit to the full 12-month scar care process
Your skin has an extraordinary capacity to heal. Give it the right conditions, and the results will speak for themselves.
👉 Book Your Free Mole Removal Consultation at TMSC Today
References
- Mustoe, T. A., Cooter, R. D., Gold, M. H., Hobbs, F. D., Ramelet, A. A., Shakespeare, P. G., … & Ziegler, U. E. (2002). International clinical recommendations on scar management. Plastic and Reconstructive Surgery, 110(2), 560–571.
- Leventhal, D., Furr, M., & Reiter, D. (2006). Treatment of keloids and hypertrophic scars: a meta-analysis and review of the literature. Archives of Facial Plastic Surgery, 8(6), 362–368.
- Atiyeh, B. S., Costagliola, M., & Hayek, S. N. (2007). Effect of silver on burn wound infection control and healing: review of the literature. Burns, 33(2), 139–148.
- Tandara, A. A., & Mustoe, T. A. (2004). Oxygen in wound healing — more than a nutrient. World Journal of Surgery, 28(3), 294–300.
- Winter, G. D. (1962). Formation of the scab and the rate of epithelization of superficial wounds in the skin of the young domestic pig. Nature, 193(4812), 293–294.
- Gold, M. H. (1994). A controlled clinical trial of topical silicone gel sheeting in the treatment of hypertrophic scars and keloids. Journal of the American Academy of Dermatology, 30(3), 506–507.